Ketamine offers rapid relief for a variety of diagnoses. Whether we are treating major depression, the depressed phase of bipolar disorder (bipolar depression), postpartum depression, anxiety, post-traumatic stress disorder (PTSD), addiction, obsessive compulsive disorder (OCD), or pain syndromes such as fibromyalgia and complex regional pain syndrome (CRPS), ketamine provides some immediate benefit. Getting a break from pain or intrusive thoughts allows a bit of “breathing room”. The ultimate promise of ketamine therapy, however, is long-term, long-lasting change. That’s why treatment planning here at Satori Integrative Medicine Clinic includes working with mental health providers, physical therapists, and other health care professionals to help our patients make the neurlogical changes that lead to sustained improvement. Let’s explore how ketamine treatment works.
How Ketamine Treatment Works in the Brain
“How does ketamine work?” is one of the most common questions we are asked when people inquire about treatment here at Satori Integrative Medicine Clinic. Our response is generally,
“Well, it allows you to change the way your brain and nervous system work. How much detail do you want?”
To be honest, neither we, nor the many scientists studying ketamine pharmacology, completely understand what turns out to be a very complex mechanism. The science behind how ketamine works is evolving every day. The way we describe it at an observable human-scale level is that it does two things:
Nervous System Reset
First, it causes a “reset” of the nervous system – something similar to what you get from a hard reset on an electronic device. We know from functional MRI evaluations that ketamine increases activity across large areas of the brain. We think that this means some communication and connectivity is occurring across parts of the nervous system that have not been “talking” to each other. For example, in Major Depressive Disorder (MDD), where connectivity is disrupted, ketamine infusion therapy largely normalizes connections within 24 hours.
Neuroplasticity
Second, ketamine creates a brain environment that promotes neuroplasticity for about 72 hours after an infusion. In simple terms, these conditions mean that your nervous system can learn and unlearn things more easily than at other times. What that means in reality is that the 2 or 3 days after treatment is the optimal time to be doing important work aimed at changing your brain – mindfulness, targeted therapy like EMDR for PTSD, or directed physical therapy for a pain syndrome. This is the time to practice the behaviors and activities you want to create or reinforce in your life.
We know ketamine works. Exactly how is complicated and still being sorted out.
For example, we know that within 24 hours of a ketamine infusion, scientists using functional MRI and other sophisticated technology can see changes to parts of the brain we know play important roles in PTSD and depression (and likely other processes as well). Alterations in the prefrontal cortex, the amygdala, and the hippocampus all indicate rapid neuroplasticity. These same scientists showed that improvement in the symptoms of depression correlated strongly with these changes.
What causes these changes to happen is still a bit mysterious. Several research labs are looking at different things ketamine seems to do at the cellular and subcellular level. The ketamine molecule and its immediate metabolites (think of these as the compounds our bodies create by processing ketamine) work through dozens of mechanisms. Here are some of the most important examples of how ketamine treatment works…
-
Ketamine is an NMDA receptor antagonist
The most well-known and frequently discussed mechanism for ketamine’s many actions is through it’s effect on the NMDA receptor. Ketamine temporarily blocks this important channel in nerve cells that is critical for how these cells respond to stimulation (especially being overstimulated), learning, memory, pain, and neuroplasticity. For depression, at least part of the way ketamine works is by changing how the NMDA receptor responds to glutamate and glycine.
-
Ketamine and some of its metabolites are active at opioid and cannabinoid receptors
These sites are really important for how we experience physical and emotional content. For example, “runners high” is thought to result from endorphins and endocannabinoids acting on these receptors. We know that blocking opioid receptors interferes with the antidepressant effects of ketamine but we don’t know exactly how.
-
Ketamine is a potent anti-inflammatory
Ketamine it works by decreasing some stress hormones and pro-inflammatory compounds like IL-6 & TNF-α. This action is really important for modulating pain but also likely contributes to some of the immediate effects on mood.
-
Ketamine promotes new neural pathways
Ketamine and its metabolites create a lot of change in nerve cells through different molecular pathways like mTOR, AMPA, and eEF2. These substances all promote the production of a protein called Brain-Derived Neurotrophic Factor (BDNF) which, in turn, plays a critical role in the growth, health, and function of neurons. Encouraging formations of new cells, new connections, and new patterns of response.
-
Ketamine alters DNA transcription in nerve cells
Long term effectiveness of ketamine seems to require a protein called Methyl CpG binding protein 2 (MeCP2) that increases growth of nerve cell spines (those little spindly branches you see at the ends of the nerves) and changes which parts of the cellular DNA are getting used to make proteins. We don’t know exactly how this works but we know that it is necessary for ketamine to have a lasting antidepressant effect.
-
Ketamine changes the behavior of astrocytes
Astrocytes are cells in the nervous system that essentially care for the nerve cells. Astrocytes manage the environment in the central nervous system: cleaning up neurotransmitters, supplying sources of energy, providing structural support, responding to injury and disease. Ketamine induces neuroplasticity in astrocytes, just like it does in neurons. These changes are important to the antidepressant effects, likely through changes in BDNF availability as well as other mechanisms we have yet to discover.
-
Ketamine alters the gut microbiome
Some evidence suggests that the antidepressant action of ketamine can be attributed to its effects on the microbiome. The brain-gut-microbiota axis has a role in the pathophysiology of depression through its involvement in the immune system, endocrine system, and vagus nerve. The gut microbiome also influences BDNF levels (see #4).
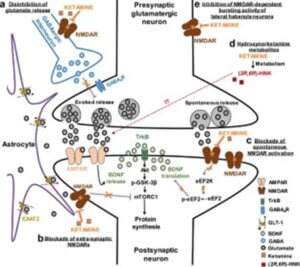
The diagram below is a good visual representation of ketamine’s mechanism of action. It looks complicated, yet shows only a few of the ways we know about how ketamine treatment works.
Image credit: https://www.nature.com/articles/s41386-023-01629-w#Sec6
The Counseling Component
Even though we don’t know all of the details around ketamine pharmacology, we do know that it is very effective for treating many different symptoms. We know that it works quickly and that it works for more than 70% of patients with treatment refractory depression. We know that people get near-immediate relief from suicidal thoughts. We also know that, in the right set and setting, ketamine can “rewire” the brain, resulting in lasting change. Good quality therapy in conjunction with ketamine infusions can make that rewiring process more conscious, effective and sustainable.
References
- Ketamine and pharmacological imaging: use of functional magnetic resonance imaging to evaluate mechanisms of action https://pmc.ncbi.nlm.nih.gov/articles/PMC5687297/
- Ketamine in Bipolar Disorder: A Review – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7670087/
- Frontiers | Psychedelics and Neuroplasticity: A Systematic Review Unraveling the Biological Underpinnings of Psychedelics (frontiersin.org) – https://www.frontiersin.org/journals/psychiatry/articles/10.3389/fpsyt.2021.724606/full
- Behind the Buzz: How Ketamine Changes the Depressed Patient’s Brain – https://www.scientificamerican.com/article/behind-the-buzz-how-ketamine-changes-the-depressed-patients-brain/
- The endogenous opioid system in the medial prefrontal cortex mediates ketamine’s antidepressant-like actions – https://www.nature.com/articles/s41398-024-02796-0



Recent Comments